LINX: Magnetic Sphincter Augmentation
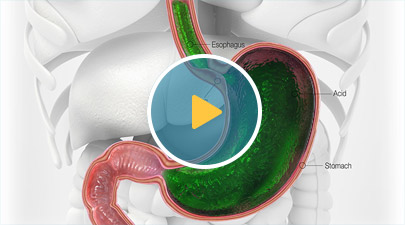
LINX is easy to understand and love because it is simple. LINX is a small, flexible ring of magnets, that opens to allow food and liquid down, then closes to prevent stomach contents from moving up. It augments the Lower Esophageal Sphincter helping to prevent reflux at the source. It requires no alteration to the stomach unlike a Nissen Fundoplication or Toupet procedure. It is placed with a minimally invasive technique with small incisions that allow most patients to go home on the day of the operation. Patients are usually able to resume normal activities within a few days post operatively. Furthermore, patients are encouraged to resume a normal diet within 2 days after the procedure.
The LINX device was approved by the FDA in 2012 after multiple 5 year clinical trial studies. It has been shown to be a safe, effective and durable surgical alternative for treating GERD. The majority of patients (over 85%), in these clinical trials were able to discontinue their PPI usage, eliminate heartburn symptoms and regurgitation with overall improved quality of life.
Although there have been over 4,000 of these devices implanted, the number of surgeons world wide who have been trained to perform this procedure is limited.
Dr. Shachner is one of the few surgeons in Florida who has both the training and experience to perform this procedure. He has safely placed over 30 of the LINX devices in the first year that he had completed his training.

Nissen Fundoplication
The Nissen Fundoplication is a minimally invasive procedure in which a patient’s stomach is wrapped around the lower portion of the esophagus, called the LES (Lower Esophageal Sphincter).
This wrap attempts to recreate the valve at the LES that has begun to fail and is contributing to the patient’s reflux. Patients will need to resume a mostly liquid diet for a few weeks post-surgery.
This is an excellent procedure that Dr. Shachner has extensive experience performing with excellent results.
For many patients, the LINX procedure has supplanted this operation.

Hiatal Hernia Repair:
A hiatal hernia repair is warranted when a patients crural muscles (the muscles that support the esophagus as it passes through the diaphragmatic hiatus) have separated and are no longer supporting the esophagus at the area of the hiatus and a portion or sometimes all of the stomach enters the chest.
In a hiatal hernia repair, the physician will use sutures to bring these muscles back together after returning the stomach to the abdomen.
Very often, a hiatal hernia repair is needed with either the LINX procedure or the Nissen Fundoplication procedure.
In addition to a weakened LES, the existence of a hiatal hernia is a contributor to a patient’s reflux so it is important that this is fixed at the time of surgery.

TIF/Esophyx:
TIF or Transoral Incisionless Fundoplication is an endoscopic procedure that is performed using an endoscope through the mouth.
During the TIF procedure, the surgeon attempts to reconstruct the anti-reflux barrier.
Most patients go home the day after surgery and resume normal activities within a few days.
Heller Myotomy:
Sometimes after the preoperative workup studies have been performed, we find that a patient has another condition called Achalasia. Achalasia is a disease in which it becomes difficult for a patient to pass food or drink from the esophagus into the stomach.
This condition may warrant a procedure called Heller Myotomy. During this procedure, the surgeon will cut and separate the esophageal sphincter muscle to relieve some of the pressure that is being exerted. Dr. Shachner will also do a partial Fundoplication or wrapping of the stomach over the esophagus at the time of the Heller Myotomy procedure to prevent post procedure reflux.



Robotic Surgery:
Robotic surgery is a form of minimally invasive surgery that allows complex procedures to be completed safely and with a small incision.
Patients are often discharged home on the day of their procedure.